Research Poster
(P08) Comparison of Zirconia vs. Titanium Dental Implants: Material Properties, Biological Response, Esthetics & Clinical Applications

Ibrahim Nasr, Dental Student
Dental Student
Lincoln Memorial University College of Dental Medicine
Knoxville, Tennessee, United States
Speaker(s)
Purpose of the Study: Titanium has long been considered the gold standard in implant dentistry due to its predictable osseointegration, mechanical strength, and survival rates exceeding 95% (Morena et al., 2024; Osman & Swain, 2015). However, increasing patient demand for metal-free, tooth-colored alternatives has driven interest in zirconia implants. Zirconia offers potential advantages in esthetics, soft tissue integration, and reduced plaque accumulation, making it attractive for anterior esthetic zones and for patients with metal sensitivities (Sales et al., 2023; Chile et al., 2023). Despite these benefits, zirconia remains limited by material brittleness, fewer prosthetic options, and less long-term data compared with titanium (Fernandes et al., 2022; Duan et al., 2023). Importantly, because implant dentistry is a restorative discipline with a surgical component, clinicians must consider that failure of zirconia restorative components may necessitate implant removal. Such removal carries higher morbidity and surgical complexity, potentially converting an otherwise straightforward restorative case into a compromised or complicated treatment scenario.
Methods: A structured review of the current literature was conducted, emphasizing systematic reviews, meta-analyses, and randomized controlled trials. Eight systematic reviews/meta-analyses and one critical materials review were included (Morena et al., 2024; Padhye et al., 2023; Fernandes et al., 2022; Sales et al., 2023; Duan et al., 2023; Haimov et al., 2023). Data were extracted for mechanical properties, biological behavior, esthetic outcomes, implant survival, and clinical applications. Comparative analysis highlighted site-specific indications and limitations of each implant type.
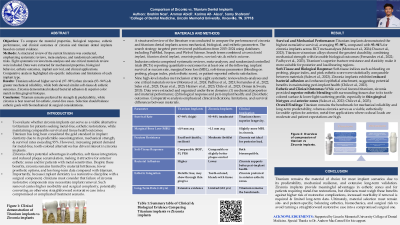
Results: Titanium implants consistently demonstrated higher survival rates and lower MBL compared to zirconia across RCT meta-analyses (Duan et al., 2023; Morena et al., 2024). Pooled survival data reported ~97–98% for titanium and ~93–94% for zirconia, with titanium–zirconium alloys achieving the highest survival (Fernandes et al., 2022; Haimov et al., 2023; Padhye et al., 2023). Soft tissue outcomes, including bleeding on probing, plaque index, and pink esthetic score, were statistically similar between Ti and Zr (Sales et al., 2023; Morena et al., 2024). Zirconia implants demonstrated lower bacterial adhesion and potentially improved peri-implant health (Chile et al., 2023). Mechanically, titanium remains superior, offering greater fracture resistance, toughness, and prosthetic versatility (Osman & Swain, 2015), while zirconia is more brittle and less adaptable to complex prosthetic designs (Duan et al., 2023). Esthetically, zirconia’s tooth-colored, metal-free nature makes it especially advantageous in anterior and thin gingival biotypes (Chile et al., 2023; Sales et al., 2023).
Conclusion: Titanium remains the material of choice for most implant scenarios due to its predictability, mechanical resilience, and extensive long-term validation (Morena et al., 2024; Duan et al., 2023). Zirconia implants provide meaningful advantages in esthetic zones and for patients requiring metal-free restorations, but clinicians must weigh these benefits against higher risk of restorative complications, increased morbidity if removal is required, and limited long-term data (Haimov et al., 2023; Fernandes et al., 2022). Ultimately, material selection must remain site- and patient-specific, balancing esthetics, biomechanics, and surgical risk to avoid turning a straightforward restorative case into a compromised surgical one.
Articles: Morena D, Leitão-Almeida B, Pereira M, Resende R, Fernandes JCH, Fernandes GVO, Borges T. Comparative clinical behavior of zirconia versus titanium dental implants: a systematic review and meta-analysis of randomized controlled trials. J Clin Med. 2024;13(15):4488. doi:10.3390/jcm13154488
Padhye NM, Calciolari E, Zuercher AN, Tagliaferri S, Donos N. Survival and success of zirconia compared with titanium implants: a systematic review and meta-analysis. Clin Oral Investig. 2023;27(11):6279-6290. doi:10.1007/s00784-023-05242-5
Chile J, Dolores A, Espinoza-Carhuancho F, Alvitez-Temoche D, Munive-Degregori A, Barja-Ore J, Mayta-Tovalino F. Zirconia dental implants as a different alternative to titanium: a literature review. J Int Soc Prev Community Dent. 2023;13(5):357-364. doi:10.4103/jispcd.JISPCD_104_23
Osman RB, Swain MV. A critical review of dental implant materials with an emphasis on titanium versus zirconia. Materials. 2015;8(3):932-958. doi:10.3390/ma8030932
Fernandes PRE, Otero AIP, Fernandes JCH, Nassani LM, Castilho RM, de Oliveira Fernandes GV. Clinical performance comparing titanium and titanium–zirconium or zirconia dental implants: a systematic review of randomized controlled trials. Dent J (Basel). 2022;10(5):83. doi:10.3390/dj10050083
Sales PHH, Barros AWP, Oliveira-Neto OB de, Lima FJC de, Carvalho AAT de, Leão JC. Do zirconia dental implants present better clinical results than titanium dental implants? A systematic review and meta-analysis. J Stomatol Oral Maxillofac Surg. 2023;124:101324. doi:10.1016/j.jormas.2022.10.013
Duan C, Ye L, Zhang M, Yang L, Li C, Pan J, Wu Y, Cao Y. Clinical performance of zirconium implants compared to titanium implants: a systematic review and meta-analysis of randomized controlled trials. PeerJ. 2023;11:e15010. doi:10.7717/peerj.15010
Haimov E, Sarikov R, Haimov H, Juodzbalys G. Differences in titanium, titanium–zirconium, and zirconia implant treatment outcomes: a systematic literature review and meta-analysis. J Oral Maxillofac Res. 2023;14(3):e1. doi:10.5037/jomr.2023.14301
Books: Morena D, Leitão-Almeida B, Pereira M, Resende R, Fernandes JCH, Fernandes GVO, Borges T. Comparative clinical behavior of zirconia versus titanium dental implants: a systematic review and meta-analysis of randomized controlled trials. J Clin Med. 2024;13(15):4488. doi:10.3390/jcm13154488
Padhye NM, Calciolari E, Zuercher AN, Tagliaferri S, Donos N. Survival and success of zirconia compared with titanium implants: a systematic review and meta-analysis. Clin Oral Investig. 2023;27(11):6279-6290. doi:10.1007/s00784-023-05242-5
Chile J, Dolores A, Espinoza-Carhuancho F, Alvitez-Temoche D, Munive-Degregori A, Barja-Ore J, Mayta-Tovalino F. Zirconia dental implants as a different alternative to titanium: a literature review. J Int Soc Prev Community Dent. 2023;13(5):357-364. doi:10.4103/jispcd.JISPCD_104_23
Osman RB, Swain MV. A critical review of dental implant materials with an emphasis on titanium versus zirconia. Materials. 2015;8(3):932-958. doi:10.3390/ma8030932
Fernandes PRE, Otero AIP, Fernandes JCH, Nassani LM, Castilho RM, de Oliveira Fernandes GV. Clinical performance comparing titanium and titanium–zirconium or zirconia dental implants: a systematic review of randomized controlled trials. Dent J (Basel). 2022;10(5):83. doi:10.3390/dj10050083
Sales PHH, Barros AWP, Oliveira-Neto OB de, Lima FJC de, Carvalho AAT de, Leão JC. Do zirconia dental implants present better clinical results than titanium dental implants? A systematic review and meta-analysis. J Stomatol Oral Maxillofac Surg. 2023;124:101324. doi:10.1016/j.jormas.2022.10.013
Duan C, Ye L, Zhang M, Yang L, Li C, Pan J, Wu Y, Cao Y. Clinical performance of zirconium implants compared to titanium implants: a systematic review and meta-analysis of randomized controlled trials. PeerJ. 2023;11:e15010. doi:10.7717/peerj.15010
Haimov E, Sarikov R, Haimov H, Juodzbalys G. Differences in titanium, titanium–zirconium, and zirconia implant treatment outcomes: a systematic literature review and meta-analysis. J Oral Maxillofac Res. 2023;14(3):e1. doi:10.5037/jomr.2023.14301
Methods: A structured review of the current literature was conducted, emphasizing systematic reviews, meta-analyses, and randomized controlled trials. Eight systematic reviews/meta-analyses and one critical materials review were included (Morena et al., 2024; Padhye et al., 2023; Fernandes et al., 2022; Sales et al., 2023; Duan et al., 2023; Haimov et al., 2023). Data were extracted for mechanical properties, biological behavior, esthetic outcomes, implant survival, and clinical applications. Comparative analysis highlighted site-specific indications and limitations of each implant type.
Results: Titanium implants consistently demonstrated higher survival rates and lower MBL compared to zirconia across RCT meta-analyses (Duan et al., 2023; Morena et al., 2024). Pooled survival data reported ~97–98% for titanium and ~93–94% for zirconia, with titanium–zirconium alloys achieving the highest survival (Fernandes et al., 2022; Haimov et al., 2023; Padhye et al., 2023). Soft tissue outcomes, including bleeding on probing, plaque index, and pink esthetic score, were statistically similar between Ti and Zr (Sales et al., 2023; Morena et al., 2024). Zirconia implants demonstrated lower bacterial adhesion and potentially improved peri-implant health (Chile et al., 2023). Mechanically, titanium remains superior, offering greater fracture resistance, toughness, and prosthetic versatility (Osman & Swain, 2015), while zirconia is more brittle and less adaptable to complex prosthetic designs (Duan et al., 2023). Esthetically, zirconia’s tooth-colored, metal-free nature makes it especially advantageous in anterior and thin gingival biotypes (Chile et al., 2023; Sales et al., 2023).
Conclusion: Titanium remains the material of choice for most implant scenarios due to its predictability, mechanical resilience, and extensive long-term validation (Morena et al., 2024; Duan et al., 2023). Zirconia implants provide meaningful advantages in esthetic zones and for patients requiring metal-free restorations, but clinicians must weigh these benefits against higher risk of restorative complications, increased morbidity if removal is required, and limited long-term data (Haimov et al., 2023; Fernandes et al., 2022). Ultimately, material selection must remain site- and patient-specific, balancing esthetics, biomechanics, and surgical risk to avoid turning a straightforward restorative case into a compromised surgical one.
Articles: Morena D, Leitão-Almeida B, Pereira M, Resende R, Fernandes JCH, Fernandes GVO, Borges T. Comparative clinical behavior of zirconia versus titanium dental implants: a systematic review and meta-analysis of randomized controlled trials. J Clin Med. 2024;13(15):4488. doi:10.3390/jcm13154488
Padhye NM, Calciolari E, Zuercher AN, Tagliaferri S, Donos N. Survival and success of zirconia compared with titanium implants: a systematic review and meta-analysis. Clin Oral Investig. 2023;27(11):6279-6290. doi:10.1007/s00784-023-05242-5
Chile J, Dolores A, Espinoza-Carhuancho F, Alvitez-Temoche D, Munive-Degregori A, Barja-Ore J, Mayta-Tovalino F. Zirconia dental implants as a different alternative to titanium: a literature review. J Int Soc Prev Community Dent. 2023;13(5):357-364. doi:10.4103/jispcd.JISPCD_104_23
Osman RB, Swain MV. A critical review of dental implant materials with an emphasis on titanium versus zirconia. Materials. 2015;8(3):932-958. doi:10.3390/ma8030932
Fernandes PRE, Otero AIP, Fernandes JCH, Nassani LM, Castilho RM, de Oliveira Fernandes GV. Clinical performance comparing titanium and titanium–zirconium or zirconia dental implants: a systematic review of randomized controlled trials. Dent J (Basel). 2022;10(5):83. doi:10.3390/dj10050083
Sales PHH, Barros AWP, Oliveira-Neto OB de, Lima FJC de, Carvalho AAT de, Leão JC. Do zirconia dental implants present better clinical results than titanium dental implants? A systematic review and meta-analysis. J Stomatol Oral Maxillofac Surg. 2023;124:101324. doi:10.1016/j.jormas.2022.10.013
Duan C, Ye L, Zhang M, Yang L, Li C, Pan J, Wu Y, Cao Y. Clinical performance of zirconium implants compared to titanium implants: a systematic review and meta-analysis of randomized controlled trials. PeerJ. 2023;11:e15010. doi:10.7717/peerj.15010
Haimov E, Sarikov R, Haimov H, Juodzbalys G. Differences in titanium, titanium–zirconium, and zirconia implant treatment outcomes: a systematic literature review and meta-analysis. J Oral Maxillofac Res. 2023;14(3):e1. doi:10.5037/jomr.2023.14301
Books: Morena D, Leitão-Almeida B, Pereira M, Resende R, Fernandes JCH, Fernandes GVO, Borges T. Comparative clinical behavior of zirconia versus titanium dental implants: a systematic review and meta-analysis of randomized controlled trials. J Clin Med. 2024;13(15):4488. doi:10.3390/jcm13154488
Padhye NM, Calciolari E, Zuercher AN, Tagliaferri S, Donos N. Survival and success of zirconia compared with titanium implants: a systematic review and meta-analysis. Clin Oral Investig. 2023;27(11):6279-6290. doi:10.1007/s00784-023-05242-5
Chile J, Dolores A, Espinoza-Carhuancho F, Alvitez-Temoche D, Munive-Degregori A, Barja-Ore J, Mayta-Tovalino F. Zirconia dental implants as a different alternative to titanium: a literature review. J Int Soc Prev Community Dent. 2023;13(5):357-364. doi:10.4103/jispcd.JISPCD_104_23
Osman RB, Swain MV. A critical review of dental implant materials with an emphasis on titanium versus zirconia. Materials. 2015;8(3):932-958. doi:10.3390/ma8030932
Fernandes PRE, Otero AIP, Fernandes JCH, Nassani LM, Castilho RM, de Oliveira Fernandes GV. Clinical performance comparing titanium and titanium–zirconium or zirconia dental implants: a systematic review of randomized controlled trials. Dent J (Basel). 2022;10(5):83. doi:10.3390/dj10050083
Sales PHH, Barros AWP, Oliveira-Neto OB de, Lima FJC de, Carvalho AAT de, Leão JC. Do zirconia dental implants present better clinical results than titanium dental implants? A systematic review and meta-analysis. J Stomatol Oral Maxillofac Surg. 2023;124:101324. doi:10.1016/j.jormas.2022.10.013
Duan C, Ye L, Zhang M, Yang L, Li C, Pan J, Wu Y, Cao Y. Clinical performance of zirconium implants compared to titanium implants: a systematic review and meta-analysis of randomized controlled trials. PeerJ. 2023;11:e15010. doi:10.7717/peerj.15010
Haimov E, Sarikov R, Haimov H, Juodzbalys G. Differences in titanium, titanium–zirconium, and zirconia implant treatment outcomes: a systematic literature review and meta-analysis. J Oral Maxillofac Res. 2023;14(3):e1. doi:10.5037/jomr.2023.14301

